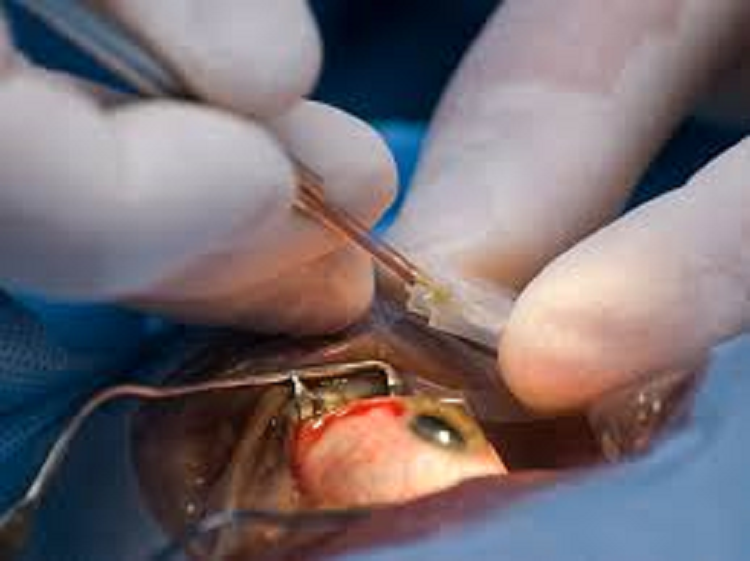
With its nationalized healthcare system, British citizens are used to healthcare rationing.
But they are paying for it in other ways.
The Times of London reports that hundreds of elderly citizens go blind each year while they wait for eye surgeries. The most recent survey by the Royal College of Ophthalmologists (RCO) discovered that despite guidance that suggested that patients not have surgery delayed, rationing of cataract surgery continued.
“The [National Health Service] has ignored instructions to end cataract treatment rationing in defiance of official guidance two years ago, a survey by the Royal College of Ophthalmologists has found,” the Times reported.
Cataract surgery is one of the most common NHS procedures with more than 400,000 such surgeries conducted each year. The National Institute for Health and Care Excellence (NICE) already stated two years ago that patients who require cataract surgery should not have to wait until they are almost blind to receive treatment. However, that situation still appears to be prevalent.
“Nothing has changed,” lamented Mike Burdon, president of the RCO. “We can’t have a situation where Nice is set up to make these decisions and [local health groups] simply say ‘we don’t like the answer’ and deprive the elderly population of the chance of a better quality of life. I’m bitterly disappointed.”
He described cataract surgery as “probably the most life-transforming procedure the NHS does.”
Helen Lee, the policy manager for the Royal National Institute of Blind People, reiterated how important cataract surgery is in a statement to the Times:
“Cataracts can have a dramatic impact on someone’s ability to lead a full and independent life, potentially stopping them from driving and increasing their chance of serious injury by falling. The Nice guidelines are in place for very good reason and make it clear that cataract surgery is highly cost-effective and should not be rationed. It is nonsensical for clinical commissioning groups to deny patients this crucial treatment.”
ADVERTISEMENT
As expected, the NHS fired back. Julie Wood, chief executive of NHS Clinical Commissioners, told the Times that “Nice guidance is not mandatory and clinical commissioners must have the freedom to make clinically led decisions that are in the best interests of both individual patients and their wider local populations,” while adding that “The NHS does not have unlimited resources.”
But this is not the first time a report on the lack of access to important eye surgeries has come out. The Telegraph reported last June that glaucoma and age-related macular degeneration patients were going blind while waiting for treatment. At that time, a survey found that up to 22 patients were going blind or partially mind every month while awaiting treatment.
The problem was also reported on as far back as 2013 with more than four in ten NHS ophthalmologists saying that they had patients who had gone blind because treatment was not administered quickly enough.
Recommended Video!
“Little House On The Prairie: Mary’s told she’s going blind”